Why study the effects of tyre noise on sleep?
Sleep serves multiple vital functions, including clearance of neural waste products that accumulate in the central nervous system during wakefulness, reducing cellular stress, synthesis of cellular components in preparation for the next period of wakefulness, consolidation of memories and restoration of cognitive performance. Epidemiologic studies consistently find associations between chronic short or interrupted sleep and negative health outcomes, particularly cardiometabolic disorders including increased risk for obesity, diabetes, hypertension, and cardiovascular disease (CVD). Importantly, there are plausible biological mechanisms linking disturbed sleep and physiological changes that precede disease, such as impaired immune function and decreased insulin sensitivity. Sleep of sufficient quality and quantity is a critical component of good health.
During sleep, the auditory system remains active and monitors the external environment for emotionally relevant signals and potential threats. Consequently, as can be related by anyone who has ever been woken up by a crying infant, a snoring partner or the late night party of a neighbour, sleep can be disrupted by noise. According to the World Health Organization, sleep disturbance carried the greatest environmental burden of disease due to traffic noise, with 903,000 healthy life years lost every year in western Europe.1 As summarised in Figure 1, there is a direct pathway from noise exposure, to sleep disturbance, to physiological stress reactions (autonomic nervous system, endocrine system), to risk factors such as changes in blood pressure, blood lipids, blood viscosity, cardiac output, blood glucose and blood clotting factors.2-5 In the long term, this may increase the risk for the development of cardiovascular disease, including hypertension, arteriosclerosis, ischemic heart disease and stroke.
There is substantial mounting evidence from experimental and epidemiological studies that nighttime noise is more relevant than daytime noise for the development of cardiovascular disease. For example, higher levels of nighttime noise have been associated with increased blood pressure,6 and there are stronger associations between road traffic noise and CVD among people who slept with open windows or whose bedroom faced the road.7 Nighttime noise may interfere with blood pressure dipping, and thereby increase cardiovascular risk 8. Long-term exposure to nighttime noise events, mainly road noise, may affect arterial stiffness, a major determinant of CVD.9 All told, both observational and experimental studies indicate that nocturnal noise can induce physiologic and metabolic changes which can result in cardiovascular risk factors,4 pointing to the critical role of the adverse effects of noise-induced sleep disruption for long-term cardiovascular health.
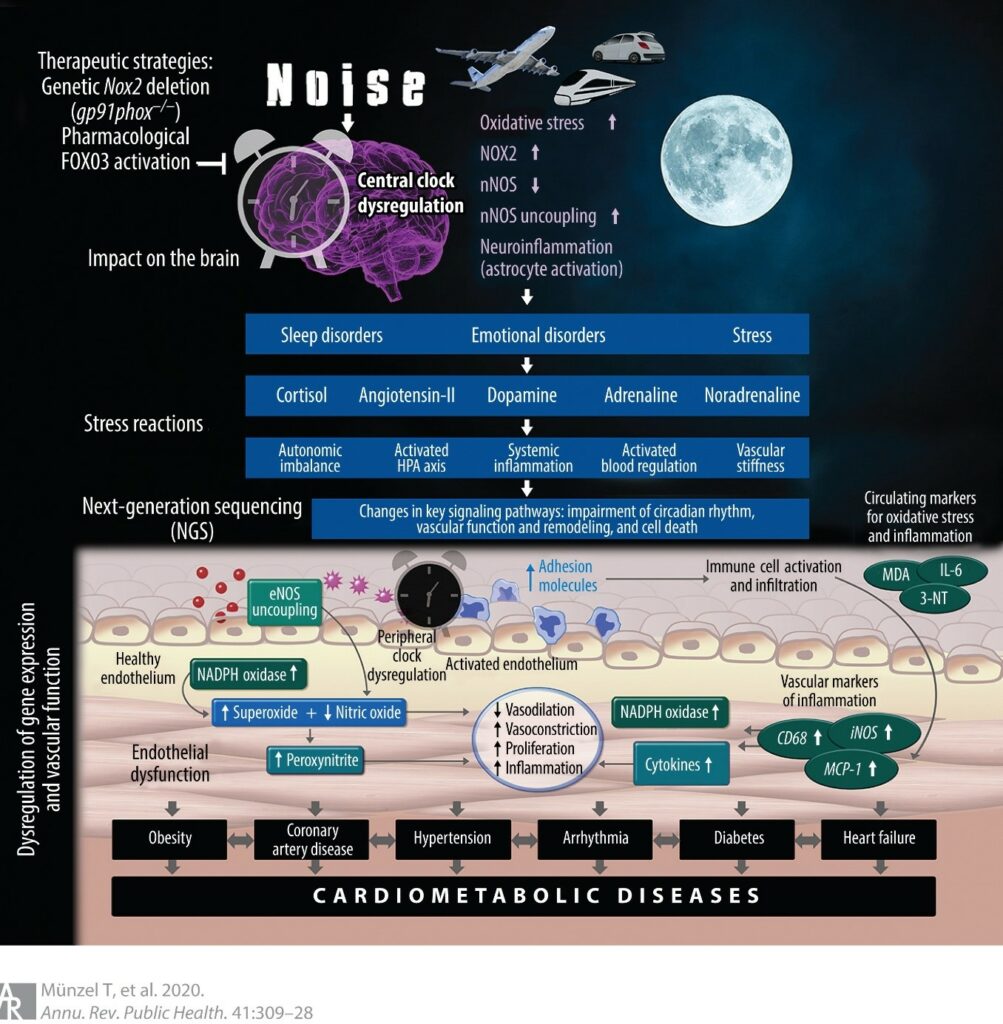 Figure: Pathophysiology of nighttime noise–induced cardiovascular and brain disease. Source: Münzel et al 2020
Figure: Pathophysiology of nighttime noise–induced cardiovascular and brain disease. Source: Münzel et al 2020
Epidemiologic studies cannot provide information on the cardiovascular impact of specific acoustical characteristics of tyre noise, therefore experimental investigations are needed. Because of the critical pathway of noise-induced sleep disturbance in the development of CVD, experimental sleep studies are crucial to understanding the physiologic impact of tyre noise on cardiovascular health. Furthermore, due to the unconscious nature of sleep, physiologic reactions are independent of an individual’s attitude, motivation, psychological sensitivity, etc. Thus experimental sleep studies allow for higher certainty in drawing conclusions on noise-induced sleep effects and long term illnesses such as CVD, compared to acute stress and cardiovascular reactions that may occur during wake but disappear during sleep.10 By including psychophysiological/biological measures during and after sleep such as metabolites and heart rate and pulse transit time, we can obtain indications of mechanisms that may lead to chronic ill health. We will therefore perform experimental investigations within LEON-T to further the effects of tyre noise on sleep and relevant cardiometabolic outcomes.
Reference:
- World Health Organization. Burden of disease from environmental noise. Quantification of healthy life years lost in Europe. 2011:101.
- Babisch W. The Noise/Stress Concept, Risk Assessment and Research Needs. Noise Health. 2002;4(16):1-11.
- Babisch W. Updated exposure-response relationship between road traffic noise and coronary heart diseases: A meta-analysis. Noise & health. Jan-Feb 2014;16(68):1-9. doi:10.4103/1463-1741.127847
- Münzel T, Gori T, Babisch W, Basner M. Cardiovascular effects of environmental noise exposure. Eur Heart J. Apr 2014;35(13):829-36. doi:10.1093/eurheartj/ehu030
- Münzel T, Kröller-Schön S, Oelze M, et al. Adverse Cardiovascular Effects of Traffic Noise with a Focus on Nighttime Noise and the New WHO Noise Guidelines. Annual Review of Public Health. 2020;41(1):309-328. doi:10.1146/annurev-publhealth-081519-062400
- Jarup L, Babisch W, Houthuijs D, et al. Hypertension and exposure to noise near airports: the HYENA study. Environ Health Perspect. Mar 2008;116(3):329-33. doi:10.1289/ehp.10775
- Babisch W, Ising H, Gallacher JE, Sweetnam PM, Elwood PC. Traffic noise and cardiovascular risk: the Caerphilly and Speedwell studies, third phase–10-year follow up. Arch Environ Health. May-Jun 1999;54(3):210-6. doi:10.1080/00039899909602261
- Haralabidis AS, Dimakopoulou K, Vigna-Taglianti F, et al. Acute effects of night-time noise exposure on blood pressure in populations living near airports. Eur Heart J. Mar 2008;29(5):658-64. doi:10.1093/eurheartj/ehn013
- Héritier H, Vienneau D, Foraster M, et al. Transportation noise exposure and cardiovascular mortality: a nationwide cohort study from Switzerland. Eur J Epidemiol. Apr 2017;32(4):307-315. doi:10.1007/s10654-017-0234-2
- Di Nisi J, Muzet A, Ehrhart J, Libert JP. Comparison of cardiovascular responses to noise during waking and sleeping in humans. Sleep. Apr 1990;13(2):108-20.
